HALLUX VALGUS
A bunion is a deformity of the base joint of the big toe. The problem is lateral deviation of the great toe so as to put a valgus deformity on the first metatarso-phalangeal joint. A deviation of 15 to 20° is considered abnormal.
This deviation upsets the biomechanics of the foot. It may cause subluxation of the first MTP joint and the great toe may even overlap the second toe.
Lateral subluxation produces a prominence on the metatarsal head (bunion) often followed by the development of a fluid filled bursa. This becomes painful as it rubs against the shoe.
Hallux Valgus right foot. The great toe deviated laterally and the 2nd toe is on of the first toe. The bunion is obvious in the medial side of the great toe.
Typical deformation of shoes from being hallux valgus (bunion)
WHAT CAUSES HALLUX VALGUS?
Contrary to common belief, high-heeled shoes with a small toe box or tight-fitting shoes do not cause hallux valgus.
However, such footwear does keep the hallux in an abducted position if hallux valgus is present, causing mechanical stretch and deviation of the medial soft tissue. In addition, tight shoes can cause medial bump pain and nerve entrapment.
Hallux valgus is known to have numerous etiologies, including biomechanical, traumatic, and metabolic factors. There is higher incidence of hallux valgus in women. Footwear may account for this.
Ballet dancers spend much time up on blocks, dancing on their toes, and so they may be expected to have a high prevalence of the condition, but this is apparently not so.
Age.
Incidence increased with age, with rates of 3% in persons aged 15-30 years, 9% in persons aged 31-60 years, and 16% in those older than 60 years.
In some cases it is associated with a joint problem such as osteoarthritis, rheumatoid arthritis, psoriatic arthropathy, gout etc.
Genetic factors have been cited with evidence to suggest familial tendencies.
SYMPTOMS
• Pain. You may then have difficulty walking due to pain.
• Inflammation and swelling at the base of the toe. This sometimes becomes infected.
• The foot may become so wide that it can be difficult to find wide enough shoes.
• You may get arthritis in the big toe.
• The second toe can become deformed.
• In severe cases, the big toe can push your second toe up out of place.
X-RAYS - MRI
The X-rays determine the extent of damage and deformity in your toe joint.
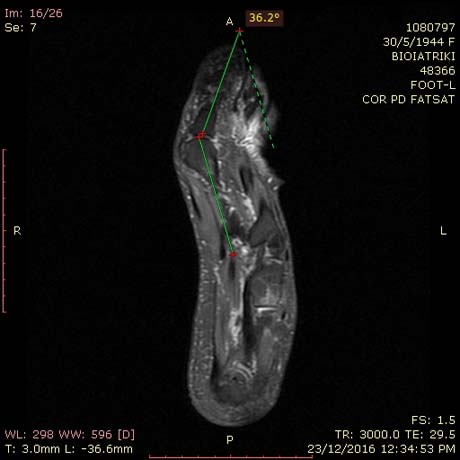
MRI is a highly accurate tool to measure the deformation of the toes and matatarsal of the foot


