PRP - PLATELET REACH PLASMA


Centrifugation of the patient's blood to isolate the plasma. In the lower vial, the red blood cells are collected and separated from the mixture.
Autologous blood products have created a growing interest for use in a number of Orthopaedic therapies. The healing effects of plasma are supported by growth factors released by platelets . These growth factors induce a healing response.
INDICATIONS
The modern method is widely used in athletic injuries (contusions muscles, ligaments ruptures, postoperative treatment after tendon sutures) in mild to moderate forms of osteoarthritis. The first results in the literature are very promising.
• Partial ligament rupture
• Tendinoses
• Muscle fiber tears
• Cartilage defect (grade I-III)
• Rotator Cuff tear
• Meniscal lesion
• Tendon suture
MECHANISM OF ACTION
Outside the bloodstream, platelets become activated and release proliferative and morphogenic proteins. These growth factors are known to be relevant for healing in a variety of tissue types. They appear to work synergistically to invoke the following benefits.
• induce proliferation and differentiation of various cell types (e.g. stem cell, osteoblast, epidermal cells)
• enhance/modulate production of collagen, proteoglycan and Tissue Inhibitor of Metalloproteinases (TIMP)
• Stimulate angiogenesis and chemotaxis
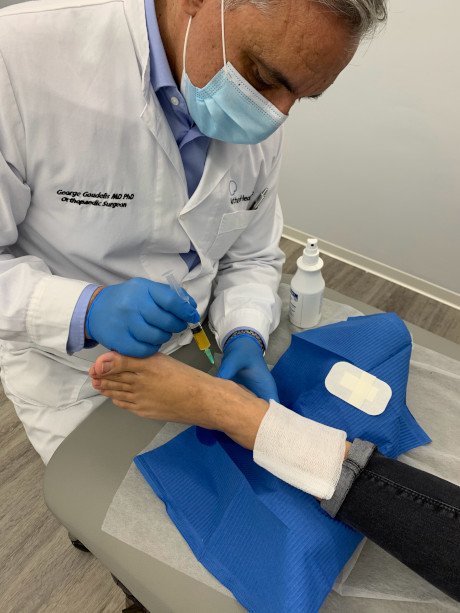
Posterior tibialis tendinitis (accessory navicular)
BIOLOGY
The average platelet concentration of whole blood is 200,000 per μL (normal range 150,000–350,000 per μL).
Platelets are small anucleated cytoplasmic fragments of megakaryocytes that are commonly thought
of as the responsible agents for hemostasis.
Although the platelet is central to the coagulation cascade, it is also essential to tissue healing. The first step of the healing process is clot formation and platelet activation.
After platelet activation, many growth and differentiation factors are released from the α-granules, which are storage units found in
platelets. Ninety-five percent of the existing factors are released within 10 minutes of clot formation, whereas the rest of the growth factors are released as they are formed over several days. In vivo and in vitro research also suggest that PRP induces overexpression of additional endogenous growth factors beyond what is contained within the platelet concentrate.
Wound healing involves an intricate process that is often categorized into three overlapping phases: inflammation, proliferation,
and remodeling. Once tissue injury occurs, a hematoma forms at the site of tissue damage, platelets adhere to exposed collagen creating a clot, and the inflammatory phase begins with activation of platelets resulting in release of growth, bioactive, and hemostatic factors.
Each factor plays a unique but codependent role in the early stages of the intrinsic and extrinsic pathways of the clotting cascade. Access to the wound site by neutrophils and macrophages occurs within hours of injury and likely serves to provide phagocytosis of tissue debris.
Within a few days of injury, the proliferative phase begins that is characterized by angiogenesis, collagen deposition, granulation tissue formation, epithelialization, and wound contraction. Finally, spanning from several weeks to months after an injury, the remodeling phase involves collagen maturation and apoptosis of excess cells.
The potential benefits of platelets reach plasma are thought to rely on the intrinsic properties and interplay between the concentrated growth factors. Some of these important growth factors include:
- platelet-derived endothelial growth factor,
- transforming growth factor–β,
- vascular endothelial growth factor,
- fibroblast growth factor,
- epidermal growth factor,
- and insulin-like growth factor -1
The complex interactions of these growth and differentiation factors, along with adhesive protein factors such as fibronectin and vitronectin, are what is responsible for the healing response; promoting the long regenerative process of chemotaxis, cell proliferation, removal of tissue debris, angiogenesis, extracellular matrix formation, osteoid production, and collagen synthesis.
METHOD OF ADMINISTRATION
The infusion of autologous plasma enriched with platelet concentrate is the cutting edge of modern therapeutics to muscle injuries (contusions and ruptures of muscles), and a degenerative bone disease (mild and moderate osteoarthritis).
The process occurs in the office or clinic.
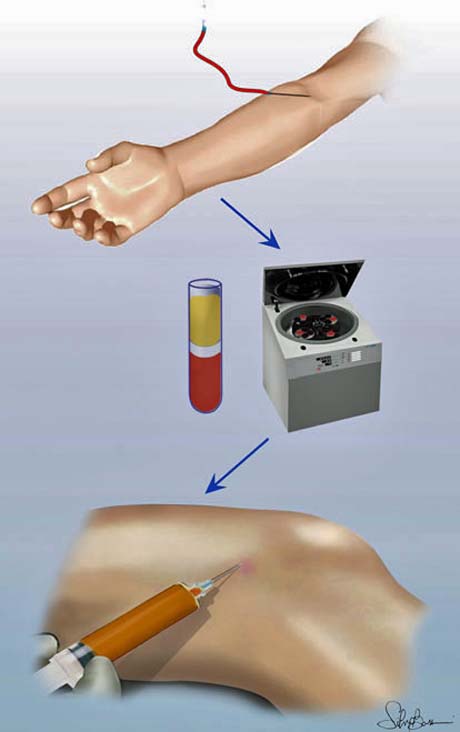
Originally done taking blood from the patient (10 cc), with a special syringe. The syringe with the patient's blood is placed in a special machine that essentially separates - isolates the patient's plasma from whole blood (over 5+10 minutes).
Received 10cc blood from the patient

Positioning the syringe with patient's blood in a special machine to separate the plasma concentrating on platelets
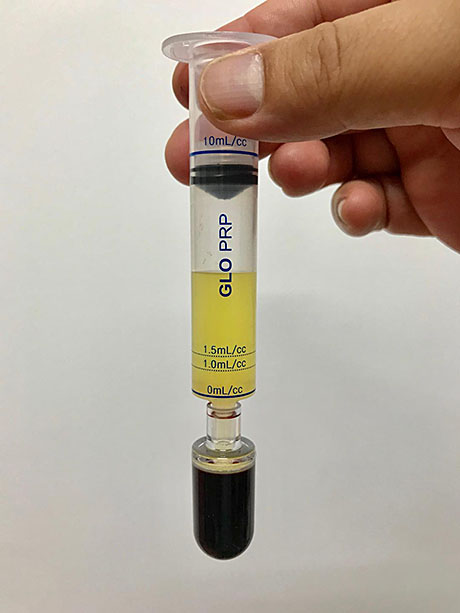
The first centrifugation is complete. The separation of platelet clear (yellow liquid). The remaining blood components collected in the lower vial (dark red liquid)
Start of the second centrifugation to clearer isolation of platelets

After the second centrifugation receive platelet rich in growth factors
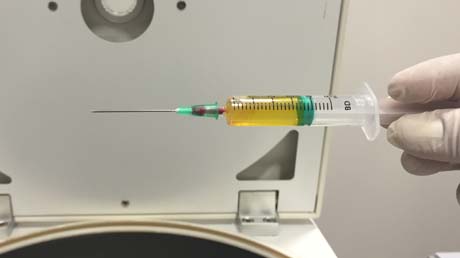
The enriched plasma captured in a separate syringe (syringe containing a yellowish liquid), are ready to be injected in the affected area
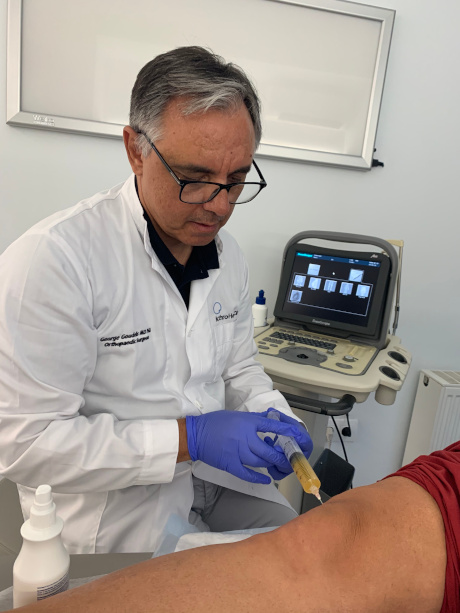
Platelet reach plasma injection in knee joint
The isolated and enriched platelet plasma injected into the affected area immediately (knee, shoulder or tendon). The procedure is painless and takes a few seconds.
Can be repeated in one week and depending on the severity of the problem may be as high as five injections.
Treatment with growth factors is now internationally one of the official methods of treating muscle injuries and tendons as well as an option for the treatment of mild to moderate joint arthritis without the occurrence of side effects or adverse reactions since it is a component of same person's suffering body.